Lublin Info Centre
Transforming radiology education with VirtuAR

Professor, could you please share with us what motivated you to establish a business in medical education using virtual reality technology?
Since 2006, I have been running a company called Entomografia that specializes in training radiologists. The idea for the business came to me after observing how radiologists are trained in top universities abroad, particularly in Belgium and the UK. I was impressed by their method of teaching radiologists to interpret medical images with specific pathologies, such as oropharyngeal cancer. To emulate this teaching method, we present participants with several MRI and CT scans of cases with different tumours and request that they diagnose the cases and submit a report on them. The lecturer then poses questions about the stage of the tumour, lymph node metastases, and possible treatment options. This approach is similar to the training provided in the best centres in Europe, and I have successfully transferred it to Poland. Together with my team, we have built the largest library of cases in Poland, covering every disease at every stage. We are proud to train over a thousand radiologists every year.
At what point did you include a virtual reality component in your training routines?
Although workshops are effective, they do not provide interactive learning. This became apparent to me when I interacted with the youngest generation of radiologists who grew up in the era of widespread smartphone use. Young people are currently used to a multitude of different stimuli. They are not inclined to focus on a longer lecture because they are used to short forms, such as Instagram Reels. For this reason, our company is using a virtual reality method. With a helmet on, trainees are free from phone calls and interfering colleagues, and all external stimuli are eliminated. They receive only the stimuli that we want them to receive. The helmet teaching method is like a computer game, in which the person moves in a three-dimensional environment and interacts with objects within it. In addition, there are haptic stimuli, e.g. if one chooses the wrong answer, the controller shakes. There is also 3D sound, which is associated with particular pathologies. Helmet learning is interactive and is linked to the participant’s full concentration.

Could you provide an example?
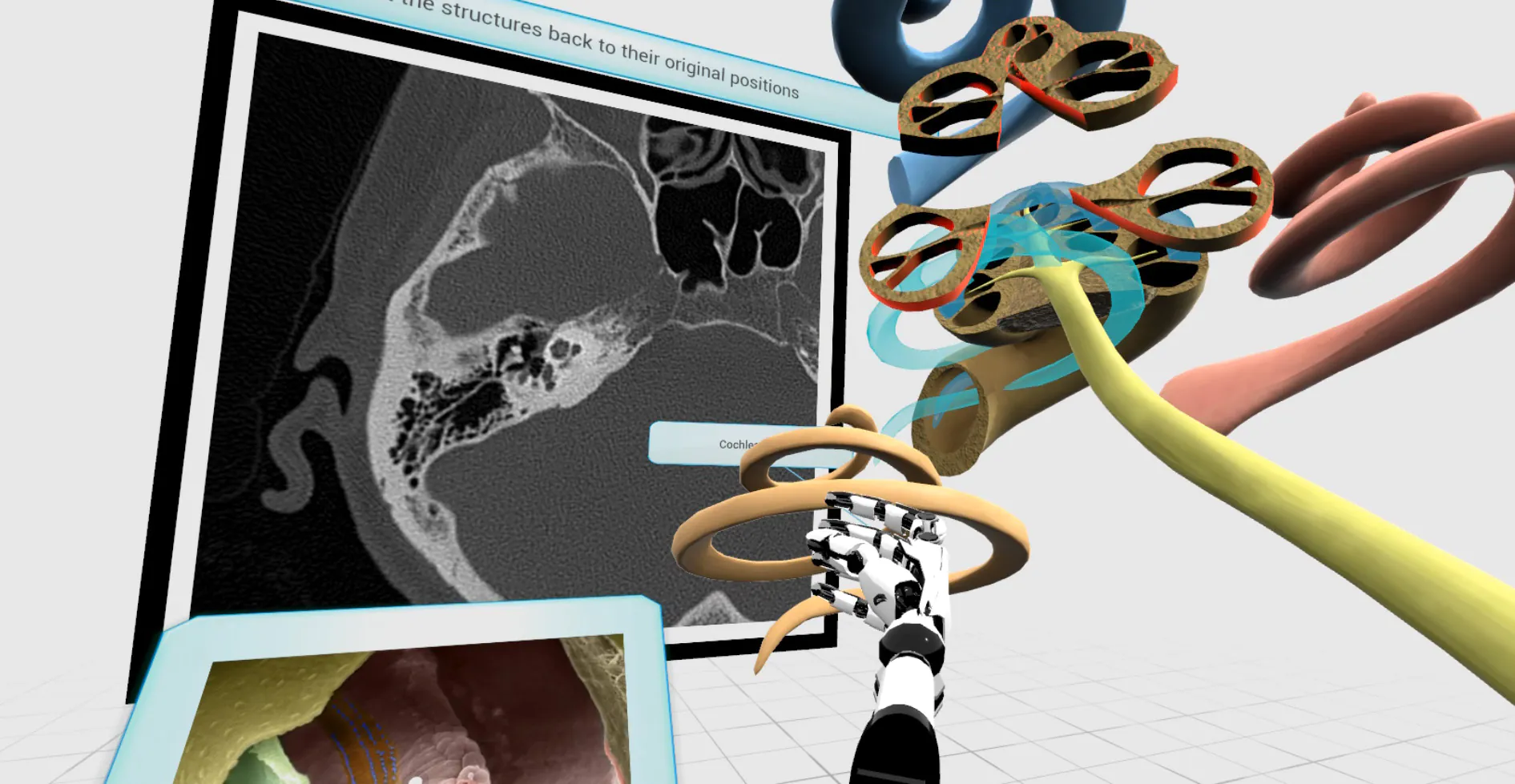
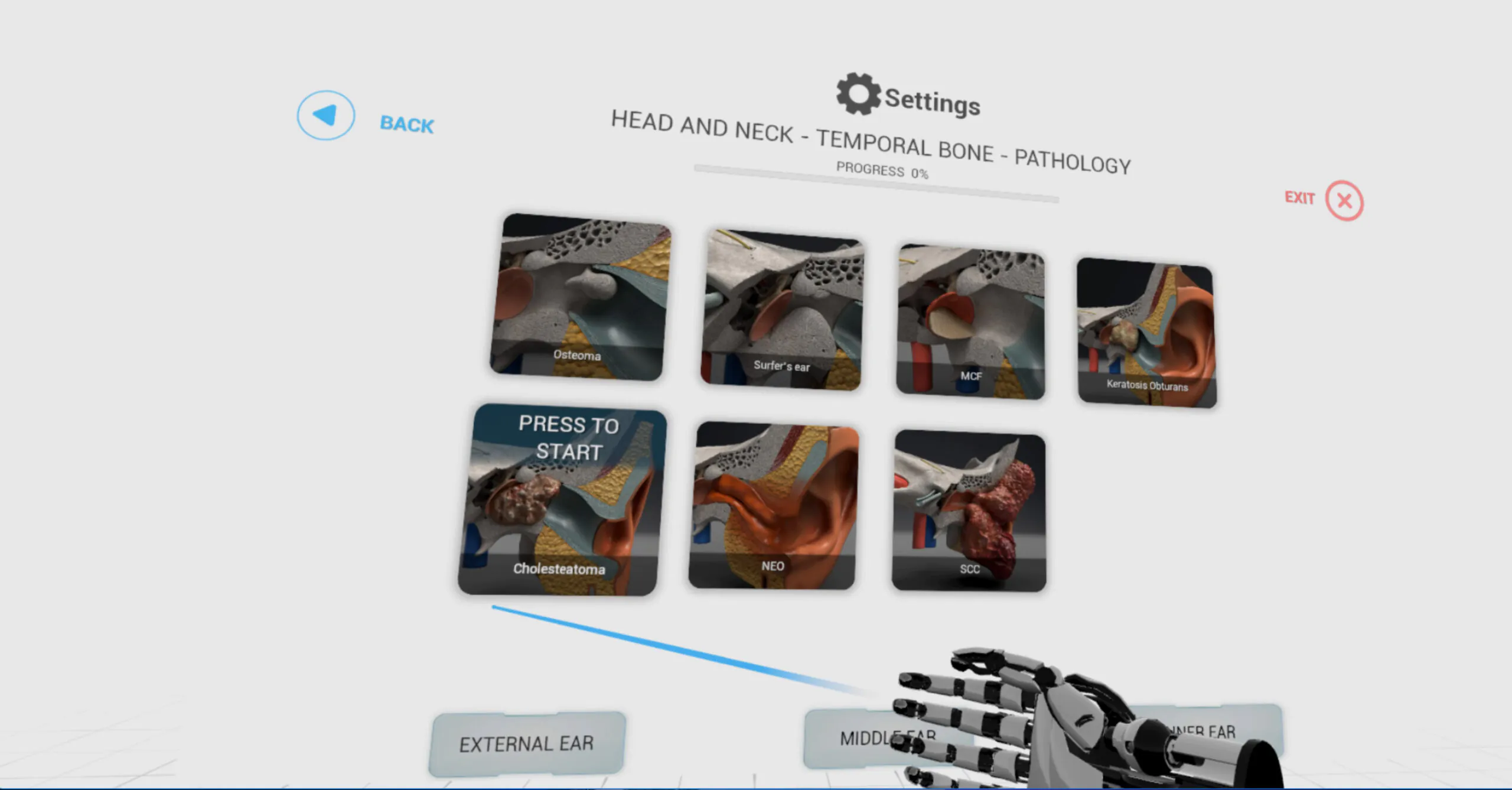
For instance, when learning about the middle ear and its parts – the malleus, incus and stapes, we use additional associations to aid memory retention. When holding the malleus, which means hammer in Latin, we hear the sound of a hammer hitting, and when holding the stapes, we hear the sound of a galloping horse. We also created images to illustrate pathologies. For instance, when teaching about cholesteatoma, a benign tumour with bone fragments that resemble snowflakes on CT images, we created an environment where snowflakes fall from the sky. Similarly, when teaching about ‘surfer’s ear’, bony outgrowths caused by exposure to seawater and wind, we transport learners to a beach in Los Angeles with surfboards stuck in the sand and the sound of the sea. This immersive learning approach turns the process into an exciting experience rather than just reading a textbook.
Who is the main audience for this training?
First and foremost, our training is designed for medical residents at various levels of advancement, as well as specialist physicians who wish to deepen or refresh their knowledge. We tailor our training to the specific level of advancement of each participant. Looking towards the nearest future, we have plans to develop virtual reality modules focused on learning about the brain, chest, prostate, and sinuses.
What was the technical development path of your solution?
My partner with whom I started this project is not only a radiologist but also a computer scientist, which is not a common combination, so he helped to create the architecture for this programme. He showed the possibility of combining a course for radiologists and virtual reality. It was an extremely long and difficult process. Furthermore, we collaborated with IT teams from several countries, including Belgium, Ukraine, Belarus, Lithuania, and Montenegro, comprising programmers, medical graphic designers, and IT specialists, at various stages of development. Initially, our program required virtual reality goggles and a computer with a robust graphics card. However, we have since reduced this to just goggles, which now cost approximately PLN 1500 (around 400 USD), and their prices continue to decline. Therefore, the cost is no longer a significant barrier. Additionally, the program can be positioned in the cloud. It is currently available in Polish and English, but we can easily provide additional language versions in the future.
What is the advantage of your solution over other learning methods?
We demonstrate the advantage of our solution over other learning methods in two ways. Firstly, by referring to the extensive scientific and medical literature of recent years, which unequivocally proves the effectiveness of virtual reality in terms of faster learning and increased memory retention in learners compared to traditional learning methods. Secondly, we conducted our own study to compare the learning efficiency of our traditional workshop method with a virtual reality prototype on a sample of 20 individuals. The results showed that learners in a virtual reality environment acquired knowledge at least four times faster and made no errors.
Are there solutions competing with those offered by Virtuar?
We have no direct competition in Poland. However, some companies specialize in creating anatomical models in virtual reality, including models designed for surgical training. These models are gradually replacing traditional dissection and autopsy classes in medical schools. Our solution, on the other hand, is unique in the field of radiology. It is not just a model, but a complete training programme that resembles a computer game. It includes levels and modules, with test questions and knowledge assessments at the end of each module.
Could you tell us about any recommendations your solution has received so far?
Our solution has received recommendations from eleven top medical centres across the globe, such as the University of Geneva, Zurich, Brescia, a significant centre for diagnostic oncology in the head and neck area, the University of Bruges, the University of Salt Lake City, the University of Chicago, and the M.D. Anderson Cancer Centre in Houston. Currently, we are actively seeking investors, including large radiology equipment manufacturers, to further develop this solution. On March 4th, I will be presenting our solution at the prestigious ECR radiology congress in Vienna, which is attended by more than 20,000 radiologists from all over the world.
How do you think artificial intelligence will affect radiology, especially with regard to advanced image recognition techniques?
I believe that eventually, artificial intelligence will take over some of the tasks performed by radiologists since algorithms already have a significant advantage in detecting pathology in CT and MRI scans. However, we still have a long way to go before these algorithms become widely available. Although AI will not completely replace doctors, human expertise will continue to be essential, and medical education will remain crucial for ensuring efficient and accurate diagnoses. To this end, we’re already planning a student version of our program, to make medical education an exciting and immersive experience.
Thank you very much for the interview.






